Obesity is a topic of discussion every day in primary care. In fact, with the recent attention that GLP-1 medications have garnered, it comes up in nearly every visit.
We’re finally having the conversation- but are we asking the right questions? Are we focused on the right outcomes? Are we really helping patients?
Obesity and weight management are big and important topics. I am going to split this post up into 3 or 4 parts so you can pick what you want to read.
Post #1 will briefly discuss:
- The magnitude of the problem in the US (spoiler alert, its BIG).
- How we define obesity (the pitfalls with our focus on BMI and measurements that are more accurate indicators of one’s health status)
- The health consequences of excess weight and obesity
Here are some of the newest stats from the CDC- if I had to guess, these are actually an understatement based on measurements that I will define later in this post.
New CDC population data from 2023 show that in 23 states more than one in three adults (35%) has obesity.
Before 2013, no state had an adult obesity prevalence at or above 35%. Currently, at least one in five adults (20%) in each U.S. state is living with obesity.
“This new data highlight the need for obesity prevention and treatment options, which start with building healthier communities where people of all ages have safe places for physical activity, and where health care and healthy food options are accessible and affordable for all,” said Karen Hacker, MD, MPH, director of CDC’s National Center for Chronic Disease Prevention and Health Promotion.
“Obesity prevention at young ages is critical, because we know that children with obesity often become adults with obesity. This is one of the reasons why we prioritize state and community investments in effective child care and family healthy weight programs.”
The problem- the obesity rate is rapidly increasing. So how do we fix it?
We need access to healthy food.
We need access to safe places to exercise in.
We need family involvement.
We need education and prevention.
How do we define overweight and obesity?
Straight from the world health organization:
Overweight is a condition of excessive fat deposits.
Obesity is a chronic complex disease defined by excessive fat deposits that can impair health.
The diagnosis of overweight and obesity is made by measuring people’s weight and height and by calculating the body mass index (BMI): weight (kg)/height² (m²). The body mass index is a surrogate marker of fatness and additional measurements, such as the waist circumference, can help the diagnosis of obesity.
- Normal weight: BMI 18.5 to 24.9
- Overweight: BMI 25 to 29.9
- Obesity: BMI 30 or greater
- Class 1 obesity: BMI 30 to 34.9
- Class 2 obesity: BMI 35 to 39.9
- Class 3 (extreme or severe obesity): BMI 40 or higher
Most BMI charts now define a BMI of 23 or higher as increased risk for people of Asian descent.
BMI is simply a measure based on height and weight, it is correlated with adiposity, though it loses accuracy very quickly in people with very high or low muscle or bone mass and fluctuates wildly with hydration status. The issue here is the use of “weight” as a measurement that defines health.
The addition of a waist circumference helps to improve the accuracy of a BMI, but what we really care about is adiposity, what is your body fat percentage? The best way to measure this is a combination of measurements to find out total body volume, body water and bone mass- I won’t go into the details, they are outside the scope of this article. But skin fold calipers, body circumference measurements and BIA (bioelectrical impedance analysis) used together can help estimate your body fat percentage within 2-4%.
Here is a link to estimate your body fat percentage based on a few different measurements:
I get it, in a clinical setting we need a quick way to provide a measurement and estimate the potential for health risk, provide guidance etc. But we need accurate measurements to do so. Here is why:

BMI is correlated to adiposity, but it is severely limited, especially at the individual level.
A brief aside on aging and body composition and why BMI may be a poor indicator of adiposity as we mature: As females and males lose estrogen and testosterone respectively, their muscle mass decreases, and fat stores increase. This is a change in body composition and tends to level off after a few years. Despite the change in body composition, some people may not even notice a significant change in weight. Here is what they do notice:
- A change in weight distribution- their pants don’t fit the same
- A change in body composition- they feel softer
- A change in metabolism- they can’t eat as much as they used to, or they start to gain weight. This is due to a change in basal metabolic rate from a decrease in muscle mass- more in this and the importance of weight training in part 3
Now that we understand how obesity is defined, the limitations of office measurements, and other ways we can estimate our body composition; It’s time to talk about the consequences of excess adiposity (fat cells).
Consequences of excess adiposity:
- Chronic inflammation
- Type 2 diabetes
- Certain cancers (uterine, ovarian, cervical, endometrial, breast, colon, rectal, liver, prostate, gallbladder and kidney)
- Sleep apnea
- Digestive issues
- Osteoarthritis
- Fatty liver disease
- Hight blood pressure
- Stroke
- Heart disease
- Hormone imbalance
If you want to know more about how obesity contributes to the development of chronic health conditions, let me know in the comments and I’ll do a separate post on the mechanism. For now, lets move on to the why.
The first step to treating obesity, is understanding the why behind it. The trick is, there are a lot of why’s and most people have more than one.
- Imbalance of energy in vs. energy out- we’re eating more calories than we’re burning. This happens for several reasons. Many of the foods and beverages commonly consumed in the US are calorie dense, and nutrient poor- lots of calories, not much nutritional value. They fill you up for the moment, but don’t provide many vitamins or minerals, they lack fiber (which provides the feeling of fullness) and are often full of simple carbohydrates which cause a spike and subsequent dip in blood sugar- leaving your hungry and looking for your next quick fix. We will talk more about macronutrients in part 3 of this post.
- Emotional eating- stress eating, boredom eating, celebratory eating, food as a reward etc. Societally, we eat for many reasons beyond fueling our bodies.
- Changes in body composition and subsequent decrease in our BMR (basal metabolic rate- the number of calories we need to sustain life and basic daily functions)- as we age, we lose muscle and our BMR decrease, you can either adjust your calories downward or actively work on maintaining or increasing muscle- most people don’t do either and end up gaining weight.
- Sedentary lifestyle- people spend much of their day at their desks, and most are not meeting exercise guidelines.
- Medical conditions that make it difficult to lose fat.
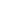
Figure 1. Percent distribution of adults aged 18 and over who met 2018 Physical Activity Guidelines for Americans for aerobic and muscle-strengthening activities: United States, 2020

Aerobic guidelines for adults recommend at least 150 to 300 minutes a week of moderate-intensity, or 75 to 150 minutes a week of vigorous-intensity, or an equivalent combination of moderate- and vigorous-intensity aerobic activity.
Muscle-strengthening guidelines for adults recommend activities of moderate or greater intensity involving all major muscle groups on 2 days a week or more.
Why is it fat loss so difficult? It turns out that weight management is affected by a number of different factors including:
- Poor sleep- impacts level of satiety (leptin) and hunger (ghrelin) hormones- lack of sleep increases your levels of ghrelin and decreases your levels of leptin. Obesity can also contribute to poor sleep, which in turn causes increasing levels of hormone dysfunction.
- Genetics- over 500 genes have been linked to obesity and may predispose an individual to weight gain, or difficulty with weight loss. The rapid rise in the obesity rate cannot be explained by genetic variation alone, but certain genes can predispose an individual to weight gaining tendencies.
- Medical conditions- PCOS, metabolic syndrome, Hashimoto’s, hormone imbalance
- Medications- certain forms of birth control, antidepressants, antipsychotics, diabetes medications, steroids, seizure medications, antihistamines (chronic use), Beta-blockers (blood pressure/ heart medication)- this is by no means a complete list, and not every medication in each category contributes to weight gain, but certainly something to consider and discuss with your doctor!
- Gut microbiome – plenty of interesting information here, I will cover this in a separate post!
- Metabolic adaptation- this is particularly difficult to navigate. Typically, when you lose weight, you do so by decreasing your caloric intake, increasing your energy expenditure, or a combination of both.
Your body adjusts to the reduced intake by decreasing the number of calories it burns in a day- it becomes more efficient with the fuel you provide it.
Additionally, there is a change in hormonal signaling with a decrease in hormones that promote satiety (fullness)- leptin, amylin, insulin, peptide YY, cholecystokinin and glucagon-like peptide-1, and an increase in hormones that increase hunger- Ghrelin - Weight loss is not uniformly fat loss- most of the time, you are losing a combination of muscle and fat. As you lose muscle, you are losing metabolically active tissue- meaning your daily caloric needs are steadily decreasing. This is also why it becomes more challenging to lose weight with each subsequent attempt- unless you’re building muscle, the process of metabolic adaptation is making it harder and harder to lose weight. More on this in another post.
If you’re still reading, I’m sure you can understand why treating obesity or excess adiposity is so challenging. Not only is it a disease with multiple causes, but it is also subject to metabolic processes that make each progressive attempt more challenging and less likely to succeed. If there is one think we know about weight loss, it is an ongoing challenge.
The first step in management is sitting down with your doctor to discuss which factors may be affecting your weight loss journey.
Ultimately, a surplus in caloric intake and sedentary lifestyles continue to be a huge part of the problem, however, it’s usually not that simple, and the best treatment plan will address multiple different factors.
On that note, I’ll end today’s post. Stay tuned for next week when we discuss natural or lifestyle management strategies for obesity including exercise, nutrition, sleep and stress management.
Sincerely,
Corsano MD- your friendly neighborhood PCP
Physiology of Weight Loss | Rethink Obesity®
Obesity and overweight (who.int)
Products – Data Briefs – Number 443 – August 2022 (cdc.gov)
Image: Body Mass Index | MannaGold







Leave a Reply